
There has been a lot of chatter in the last few weeks about the Coronavirus infection pandemic. Hundreds of thousands of people have been affected, and there have been a large number of casualties.
These are no doubt stressful times for all of us.
There have been a plethora of reports about how many people are affected on printed media. There have been even more falsehoods shared about the coronavirus infection on social media.
Many of these talk about the symptoms in short, with only some reports really covering what could happen should you get affected.
Preventive measures are the best way to limit spread and to avoid a pandemic of outstanding proportions. But what you should do to ensure you don’t get this infection is a discussion for another day.
I have a feeling you probably know about it anyway. If you don’t, I have an article for you here.
Today, I will talk about what you can expect should you get affected by the virus.
My information in this article is from reliable sources – Emcrit, New England Journal, etc – that have detailed guidelines on how doctors should manage this condition.
I will try and simplify it to the best of my ability here.
Transmission Of COVID -19
The transmission of the virus appears primarily to be through droplets floating around in the air. These droplets tend to be fairly large and can catapult to around 6 feet from the patient if they cough or sneeze.

The droplets can also be smaller in the form of aerosols (airborne) that float around in the air.
Larger droplets do not penetrate the normal surgical mask. However, to prevent getting affected by aerosols, the N-95 mask is a lot more effective than the surgical mask.
I figure you might be confused about what droplet infection and airborne infections actually are.
This is not a new confusion; it has existed previously as well during the times of Ebola virus and other viral infections.
Let me explain.
Large droplets are generated when a person coughs or sneezes. These large droplets directly land in a person’s eyes, nose or mouth.
So if you in close proximity to someone with COVID-19 infection and they sneeze, large droplets would land on your face and infect you.
Similarly, it is the large droplets that land on surfaces. When you touch these surfaces and then touch your face, nose or mouth, you can introduce these droplets into your system (hence the advice to stop touching your face).
An airborne infection is one where the virus floats around through the air long after the person coughs or sneezes. For example, if a person sneezes and then leaves a room, the virus continues to float around in the air for a while, and does not land on any surfaces.
These viruses can still be inhaled a long time after the person affected has left the vicinity. An example of an airborne illness is tuberculosis.
Currently, it is believed that the Coronavirus COVID-19 primarily spreads through droplet infection. The airborne route is still controversial, but not implausible, as published in an article in the New England Journal Of Medicine (NEJM).
Given the majority of evidence pointing towards droplet infection, the advice for the public is to use normal surgical masks.
However, in hospitals, healthcare professionals are also prone to airborne infections if they are treating COVID-19 patients, and hence they are advised to wear N-95 masks.
Furthermore, healthcare workers are involved in ventilating patients, placing oxygen masks on patients with low oxygen levels, performing cardio-pulmonary resuscitation and conducting life-saving procedures, all of which generate airborne particles.
They are directly in the line of fire.
The CDC have currently stated that in the absence of N-95 masks, regular surgical masks could be used for now.
Okay, so what about direct contact?
There are so many messages about the virus lasting on surfaces for a few hours to days. Some even go on to day that they last for a shorter duration on metal surfaces, longer on cardboard surfaces etc.
But what is the truth really?
When a person coughs or sneezes, the droplets fly out of the respiratory tract, landing on surfaces within 6 feet or so. The virus persists as ‘fomites’ in the environment.
In the NEJM paper I mentioned earlier, the research group found the virus was more stable and lived longer on plastic and stainless steel (up to 72 hours), and for a shorter duration on copper (4 hours) and cardboard surfaces (24 hours).
So if you touch these surfaces within this time frame and then touch your face, you could catch the infection.
When Do People Transmit The Infection?
You will already know that the first transmission occurred from animal to human in the Huanan Seafood And Live Animal Market in Wuhan, China. Since that index case, transmission has been between humans.
The problem lies in the fact that some people with the virus do not have symptoms. These are ‘asymptomatic’ patients, and can transmit the virus to other unsuspecting folk.
However, from the available data, it appears transmission occurs over 8 days after the illness begins and symptoms develop.
This number comes from virus culture tests, which are usually negative after 8 days of the illness in affected patients.
This information still remains vague. Some study groups have found that the virus might be transmitted over a longer duration.
Just so you also know that the basic reproduction number, or R0 (pronounced R-naught) is 2.2. This means that one person can transmit the infection to 2.2 people. The SARS virus transmitted it to 3 people.
Watch this space for more information.
So You Catch The Infection – Now What?
Once the virus enters your system, it will multiply over a period of around 4 days (may take up to 14 days), after which the symptoms begin. This period is called the incubation period.
Symptoms begin after this. There is no particular order of appearance of symptoms.
Fever is the primary symptom, accompanied by cough and breathing difficulty. Fever is seen in around 50% of cases, and the absence of fever does not rule out COVID-19 infection.
As the disease evolves (and if it becomes severe), patients may develop breathing difficulty around 6 days after exposure. They end up getting admitted around 8 days after exposure, and on a ventilator around 10 days after exposure.
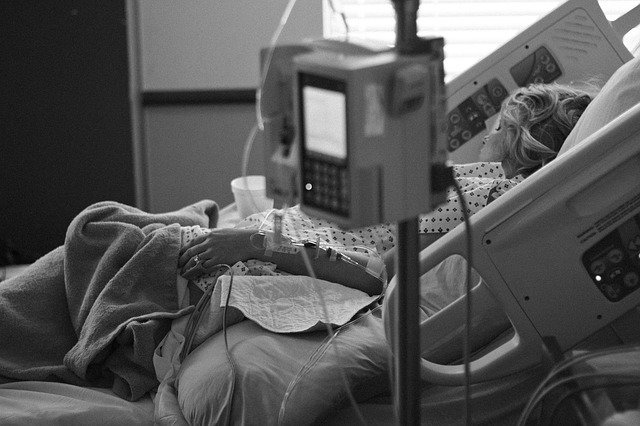
In essence, severe cases will be on a ventilator within 48 hours of admission to hospital.
Bear in mind that nearly 80% of patients have mild disease. Of the remaining 20%, only around 2 to 5% will end up with severe disease (these numbers might change in the near future).
Besides the above symptoms, around 10% of patients may develop gastrointestinal symptoms. Diarrhoea and vomiting are a part of this, and can occasionally precede the fever and breathing difficulty.
Runny nose is a rare feature, though it has been seen a few cases.
The Lungs
One problem with the COVID-19 patients is that some of them have what is called ‘silent hypoxemia’.
Hypoxemia refers to low blood oxygen levels. Normally, if we have low oxygen levels, we would breath at a faster rate in an attempt to inhale more oxygen.
A proportion of COVID-19 patients would have low oxygen levels, but would not be breathing at a fast rate.
In severe disease, a large part of the lungs will get filled with infection, leading to a ‘ground-glass’ appearance on a chest x-ray or CT scan. As the virus is filling up the lungs, there is insufficient space for oxygen to enter. This is why patients with lung involvement need oxygen treatment.
CT scans are better at picking up COVID-19 lung infections compared to chest x-rays.
The Heart
There have been reports of patients with COVID-19 infection suffering from heart attacks. The ECG changes are similar to those with a heart attack, but angiograms just show mild disease.
This is likely due to the virus attacking the heart muscle, leading to a condition called myocarditis. A troponin test will confirm whether there has been heart damage or not.
I have been talking to doctor friends of mine abroad, who are at the frontline managing COVID-19 cases actively.
Currently, when screening patients entering hospital, everyone’s temperature is checked, travel history is ascertained and oxygen levels are checked. Those with a fever and cough and low oxygen levels (below 94% – normal is 96-99%) are considered high risk and will likely be admitted.
Diagnostic Tests
Once admitted, tests will be conducted to confirm the viral infection.
Confirmation of the presence of the coronavirus infection is through an oral and nasal swab test. Orals swabs are taken before nasal swabs.
Blood tests will show a normal white blood cell count, though a specific subset of cells called lymphocytes will be low in number in up to 80% of patients.
It is rare for platelet counts to drop (seen in conditions like dengue fever), but those with a platelet count below 1 lakh carry a poorer outcome (normal platelet count is between 1.5 to 4 lakhs).
In practice, when we admit patients in hospital with suspected infections of any sort, we conduct a blood test called serum procalcitonin levels. These are generally elevated in infections.
However, in COVID-19 infections, it appears the procalcitonin levels are normal. If elevated, an alternative diagnosis may be considered.
Another blood test called C-Reactive Protein, or CRP, will be elevated. The higher it is, the poorer the outcome. A normal CRP should prompt searching for a different diagnosis.
I have already mentioned chest x-ray and CT scans as tests to determine how badly the lungs have been affected.
A small proportion of people who undergo a swab test may turn out to be negative in the early stages despite them being infected. Studies have found that up to 23% of them become positive shortly after.
This could mean that sequential testing may be needed if the clinical suspicion is high.
Treatment Options For COVID-19 – What’s Available?
There is active research ongoing with scholars and scientists testing out different tablets.

Drugs that were used to treat HIV infections are under scrutiny to evaluate their effects. Vaccines production is underway, and human trials have started. However, an effective vaccine is still months away.
Just recently, hydroxychloroquine (HCQS), a close cousin of the anti-malaria drug chloroquine, has been shown to be effective in lowering overall viral load.

Regime of administration varies, with some suggesting a loading dose of 400 mg twice daily for the first day, followed by 200 mg twice daily for 5 to 10 days, while others suggest 200 mg twice daily for 10 days.
However, do note that while the benefits have been demonstrated, they have been on a small patient group and not on a large scale.
And of course, always talk to your doctor about the real benefit versus the risks of taking the medicine. For example, if you have had certain forms of cardiac disease in the past, you may not be suitable for HCQS.
Anti-HIV drugs and other antivirals are being evaluated, and none of them are effective as of yet.
Some groups advocate adding Azithromycin, an antibiotic, to the HCQS regime. This has some effect on the COVID-19 virus, but has the added advantage of treating any super-added bacterial infections that may occur as well.
Vitamin C has gained some media attention and ‘WhatsApp forward status’ as being effective in battling the Coronavirus. But the evidence is limited.
Tablets and vaccines that were effective against H1N1 swine flu virus are not effective against COVID-19. So don’t rush to get the flu vaccine – it’s not going to protect you.
Steroids do not seem to help in early coronavirus infection, and may in fact be harmful. But in more advanced disease where the lungs are affected, they may have a limited role.
Patients who are admitted to ICU will be put on high flow oxygen delivered directly into their nostrils through a nasal cannula. This appears, so far, to be the most effective way of helping the body get enough oxygen.
More advanced therapies such as non-invasive ventilation (BiPAP) is believed to be useless.But one modality called Continuous Positive Airway Pressure, or CPAP, may have benefits, especially if delivered through a hooded device.
If these measures fail, then a tube will be inserted into the wind-pipe to ventilate the patient. Doing this can release a large number of viruses into the air, and can affect healthcare personnel greatly.
I will not go into any more detail about these ventilator modalities as it is fairly technical and out of the scope of this article.
Who Gets Better?
Around 80% of patients affected with a coronavirus infection do not need to be hospitalised and can be managed at home.
Of the hospitalised patients, up to 20% require ICU admission. Of this, around 2 to 5% die.
Antibody Testing
If you have suffered from a COVID-19 infection, then you will develop antibodies in your blood that will confirm your immunity.
It is easy to get it arranged at home, as it is a simple blood test.
You can learn more about COVID-19 antibody testing here, or you can book a test online by clicking the link here.
Staying Safe
There has been a vast amount of information sent out on different media platforms about how to prevent further spread of this virus.
Now that you know what it can do to you, please remember that you should practice preventive strategies to the ‘T’.
Wash your hands periodically. Practice social distancing. Basically, follow what the WHO and CDC say about staying safe.
Closing Remarks
You may be one of those people who feels they are invincible. Well, the virus thinks its the same.
Are you prepared to take it on a coronavirus infection, given that nearly 1 out of every 20 people who did fight it died trying? It’s up to you.
And for god’s sake, stop messing around with nature.
- Understanding Sudden Death In Young Athletes - August 18, 2025
- Coronary Angiogram – Indications, Procedure And Risks - August 18, 2025
- Gallbladder Stones – Do I Need Surgery? - April 18, 2021

